Best dry mouth products 2022
March 20, 2022 | Dry Mouth / Oral Health / Saliva / Xerostomia

Dry mouth, or low saliva production in the mouth, can be very uncomfortable. Also known as xerostomia, dry mouth can be just annoying but it can also seriously compromise your general oral health, dental health, oral hygiene and quality of life.
So which dry mouth cure is the best?
Dry mouth can be occasional or chronic and the causes are diverse. Considering each patient has different conditions and personal preferences, choosing the best treatment is an individual choice. The list below does not include all dry mouth products available. It is intended to educate dry mouth patients about their options and how each product works. However, it is best to consult your dentist or physician when choosing a xerostomia relief product.
Dry mouth relief products
As millions of people suffer from dry mouth worldwide, there are many different dry mouth products available on the market today. Xerostomia relief products, over the counter or prescribed, can be categorised into several distinctive groups:
Rinses, lozenges, gums, mints, sprays, gels, toothpastes
These products are applied topically. Some are saliva substitutes or oral lubricants and some are meant to increase saliva flow by stimulating the salivary glands. The active ingredient is one or more of the following materials:
Xylitol – a natural sugar alcohol that increases saliva flow. It may also help in preventing cavities and improving oral hygiene. Xylitol is the active ingredient in mints, gums and lozenges. It is also found in many gums and mints that are not advertised as a dry mouth product.
Betaine – produced from sugar beets. Helps with saliva production and keeps moisture in the mouth at a higher level.
Hydroxyethylcellulose – extracted from cellulose. It dissolves in water but retains a structural strength. It helps alleviate dry mouth due to its thickening and gelling qualities. Products containing this substance do not increase saliva flow but rather act as saliva substitutes.
Carboxymethylcellulose – also made out of cellulose and acts as a viscosity agent to help keep the mouth moist and lubricated.
The disadvantage of using saliva substitutes and stimulants such as lozenges and gums is that they must be used constantly and their effect is usually short term.
Natural oils
A few drops of olive oil on the tongue, for example, lubricate the mouth and may stimulate saliva production temporarily. Other natural oils may also lubricate the mouth or stimulate the salivary glands. Coconut oil, peppermint oil, spearmint oil, clove oil, eucalyptus oil, fish oil and others, each has its own characteristics.

Prescription medications
Dry mouth prescription drugs are usually prescribed to help with severe dry mouth, such as dry mouth due to Sjögren’s syndrome. They increase the secretion of fluids in the entire body – also tears and sweat – by stimulating certain nerves. These drugs encourage the salivary glands to produce more saliva. They usually contain one of two active compounds: pilocarpine or cevimeline which work on certain nerves in the body. You should only use these drugs as prescribed by your doctor as they may have side effects. For people suffering from dry mouth due to the intake of multiple different medications (polypharmacy), taking an additional medication may be counterproductive. Your physician should decide if these drugs are the proper treatment for your dry mouth.
Salagen (pilocarpine) – acts on nerves that stimulate the salivary glands to produce more saliva. Studies have shown that people using pilocarpine are twice as likely to report an improvement in the feeling of dry mouth.
Evoxac (cevimeline) – The mechanism of operation is similar to that of Salagen. Some studies have shown that Evoxac is more effective than Salagen in increasing saliva production.

Electrostimulation
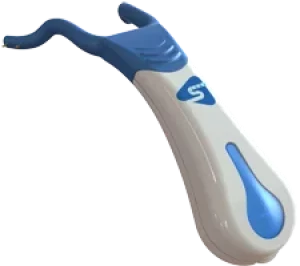
This dry mouth relief method is relatively new. The mechanism employed here is simple. By stimulating the lingual nerve with very low voltage, the salivary glands (that are regulated by this nerve) start secreting saliva naturally. Electrostimulation is performed independently by the patient, using a novel device called SaliPen®.
To stimulate the glands, SaliPen® is held under the tongue in the mouth so that its two prongs come in contact with the lingual nerve. By pressing a button on the device, a low level current is transmitted to the salivary glands. This tiny amount of electricity is not felt while it stimulates the salivary glands to produce saliva.
Electrostimulating with the SaliPen® device for 2-5 minutes each time may keep your mouth wet for hours. It is recommended to use SaliPen® up to 5 times daily. Furthermore, SaliPen® users are reporting long lasting effects. Over time, their salivary glands produce more saliva even when the device is used less frequently. A study of xerostomia treatment by electrostimulation demonstrated that the treatment is not only stimulating saliva secretion, but also regenerating the glands’ function.
Electrostimulation has no side effects, it can be applied anywhere, anytime and is only purchased once. This is why some dry mouth sufferers prefer to use SaliPen® for their dry mouth relief. In some countries, SaliPen® requires a prescription.
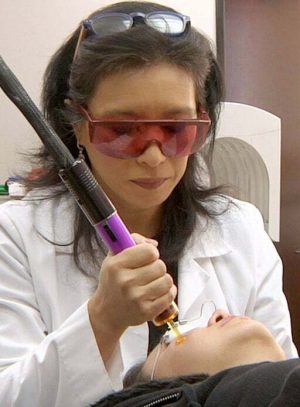
Low level laser treatment
This technique is also relatively new. By applying a low level laser beam to the salivary glands area, both in the mouth and outside, the amount of saliva secreted by the glands is increased. Over time, the same amount of treatment produced more saliva. This treatment requires special, high accuracy laser equipment and trained specialists. Access, availability and cost may be a hindering factor in attaining it.
Acupuncture
In the United States, acupuncture is considered an alternative therapy for dry mouth. Few significant scientific studies tested the efficacy of acupuncture for xerostomia patients, and the results were not conclusive in most studies. However, some studies demonstrate that acupuncture is effective as dry mouth treatment. Acupuncture is performed by inserting multiple, very fine needles at specific locations to stimulate the salivary glands. In one study conducted in Sweden, patients received 24 acupuncture sessions, lasting about 20 minutes each, over a period of four months. The results demonstrated an increased saliva flow and patients reported an objective improvement in their dry mouth feeling.
Which is the best dry mouth treatment?
The proper wording of this question is: which dry mouth treatment is the best for me?
In choosing a dry mouth treatment you should examine several factors:
- How severe is your dry mouth? Is it occasional or chronic? Temporary or permanent?
- What are your personal treatment preferences? Do you prefer medications over other treatments for example?
- Are you interested more in alleviating the symptoms of dysfunctional salivary glands or in stimulating the glands to produce more saliva?
- Consider the availability and cost of the various treatments.
With these answers at hand, consult your physician to find the best dry mouth treatment to your specific dry mouth condition.
My name is Dr. Andy Wolff, a dentist and oral medicine specialist. I have been treating and researching dry mouth and xerostomia for decades, looking for the best dry mouth cure and treatment.